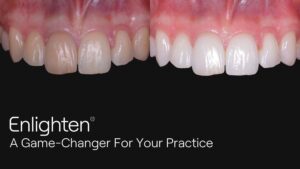
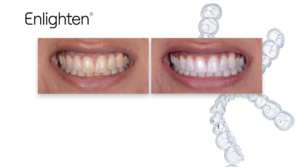
Private vs NHS dentistry
Mini Smile Makeover course demonstrators Dr. Mille Morrison and Dr. Stuart Ray break down key differences between private and NHS dentistry and the challenges that come with each sector.
Making the transition from NHS to private practice is something that crosses the mind of many dentists. Many may find it a daunting process consisting of years of training and practise in the NHS before taking on private work. With years of combined experience and knowledge, Dr. Millie Morrison and Dr. Stuart Ray are here to share their take on how to strike a balance between the two and still make progress.
Dr. Payman Langroudi: We’re here with Stuart Ray and Millie Morrison. We’ve just finished the long two day’s training dentists on composites. I wanted to talk to you about your journeys, what’s working for you guys now, where you’ve come from and where you’ve gone to. Let’s start with Stuart. Just give us a 30 second rundown on your career.
Dr. Stuart Ray: It’s been varied. I spent the first 10 to 12 years in the NHS and actually became very disillusioned about it, because it was, quite frankly, soul destroying. So thank goodness, found the private way of doing things. I wanted to concentrate on quality, not quantity.
From there I left the NHS completely and have worked in private practice ever since. Now it’s a case of concentrating on developing private skills. So nothing specialist, I’m a specialist generalist. That’s where we are today, concentrating on high quality work, looking after people and their needs and enjoying teaching as well.
Dr. Payman Langroudi: What would be your advice to someone who’s in the NHS and wants to get out of it, or wants to do more private work? What do you advise someone who’s in that situation?
Dr. Stuart Ray: I think a lot of people don’t feel that the NHS patients and NHS practices allow them to practice private work, and I don’t think that’s true. I think if you have the time to talk to your own patients, your existing patients, because you’ve already built that rapport with them and the trust with them, that’s the first place to start. It isn’t a case of jumping ship and walking out and going somewhere else. And I think that’s true for any type of practice. Concentrate on the people you’ve spent a lot of effort, a lot of time building up the goodwill and trust with.
Dr. Payman Langroudi: But if I’m a young dentist, how many years of NHS should I do before I think about that?
Dr. Stuart Ray: That’s a good question. I think in the past when I graduated people always used to say you need to be in the NHS for 10 years. I don’t see that now. I think the NHS has changed so much that the learning experience’s reduced. I think if you’re in a position where you’ve trained yourself properly, if you’re there for a few years there’s no reason why you shouldn’t be thinking of moving out much sooner.
Dr. Payman Langroudi: Sooner than twelve years?
Dr. Stuart Ray: Sooner than two years.
Dr. Payman Langroudi: Now as a counterbalance then, Millie?
Dr. Millie Morrison: I’m still in the NHS. I graduated in 2015 and I started off doing a lot of NHS work. As you just said, Stuart, I didn’t feel like I talked to my patients about private work. Maybe I didn’t think that they wanted it and they weren’t going to listen and accept the other options that I could offer, so I scaled up. I spent more time learning and slowly started approaching my patients with just a bit more openness, offering all the options and more people than I expected actually said yes. The more confidence I got speaking about prices, different techniques, being able to explain it better, meant that my patients started understanding it.
Because I’m spending more time doing private work, it’s actually allowed me to have more time to do better NHS work as well, because I’m not driven to hit that 400 UDAs in a month
Then I managed to offer better treatment more regularly. I started doing much more Invisalign and now my bread and butter is align, bleach, bond over and over again. Because I’m spending more time doing private work, it’s actually allowed me to have more time to do better NHS work as well, because I’m not driven to hit that 400 UDAs in a month. I don’t need to do that many UDAs because I’ve got the private there, which takes a lot of my time and I can spend the time of my NHS patients giving them good quality treatment, which they deserve as well.
Dr. Payman Langroudi: Your progress to becoming a teacher on Invisalign has been pretty meteoric. You just did your first full day lecture. So when you talk to dentists who are doing Invisalign, what are the common mistakes or misconceptions they’ve got? What would be some tips to accelerate someone’s Invisalign?
Dr. Millie Morrison: If I tell you a little bit more about how I progressed through the Invisalign, I think it will help to understand.
When I first did the Invisalign course it shocked me about how little control I thought I had over the whole process (and I’m a control freak, if you ask anybody that knows me, I like detail) I really want to be there. I’m not very good at delegating and a I am a bit bossy. My sister’s had that all her life. I want control, I want to know what’s going on. At first I thought that Invisalign didn’t give me that, so I did more fixed because I can control every movement. Then I spoke to my Invisalign rep, Alice, and she changed my whole view on Invisalign. I realised how much control I could get from the Invisalign system.
I started with the simple cases first, tweaking a couple of teeth, doing very simple movements, then getting my confidence up and moving to more complex cases. I now use Invisalign as part of full mouth rehabilitation. I’m doing much more difficult movements.
Dr. Payman Langroudi: So your first piece of advice is talk to your rep?
Dr. Millie Morrison: No… well actually, yes. That is a good piece of advice, because I think a lot of times we see 4 white walls and we don’t get to speak to other practitioners on a daily basis. When you have a bigger network and when you have a rep that will talk you through it and tell you what it can do and what it can’t do, then you do get a little bit more confidence, then you start meeting more people through it.
Dr. Payman Langroudi: There’s a whole lot of information out there – education the reps have, and I think it’s something that’s not often thought about, because reps have a lot of information.
Dr. Millie Morrison: As dentists we play the blame game. “It’s not my fault, it’s their fault, they haven’t approached me. Well, actually, it’s a two way street, as with any relationship, and we need to be approaching them and finding what information they can give us to allow us to then move forward. Within the first 12 months I think I’d done 65 cases. And now I’m teaching and part of the Allina consulting family and it’s great. Now I have even more support than I did when I started, and it’s just snowballing from there.
Dr. Payman Langroudi: Clinically give us some tips, or from a patient management perspective. Doing that many cases in that short period of time.
Dr. Millie Morrison: A big part of it is marketing to bring new patients in. Also what I found is that during the checkup, when I had the patient lying down, I’d be like, “oh you have some calculus or some tartar built up here. Have you ever thought about straightening the teeth to make easy to clean?” Obviously take the mirror out and I’d be like, ” yes or no?” If they had said yes, I would then approach the conversation at the end of the checkup. These and NHS patients that you’re just converting and offering treatment that they actually want, they just didn’t know you offered. A lot of my patients used to say, “oh, you do this, but my other dentist doesn’t”. Most dentists can do it.
What I do now is have a personal e-mail address, which all my Invisalign patients get
It’s just having the confidence to talk to their patients to let them know that they’re doing it. Then what I like to do or what I do now is have a personal e-mail address, which all my Invisalign patients get.
The next day after the appointment I send them an email saying: ‘thank you very much. It was nice to meet you, I hope you found it useful. Here’s my personal email address. Please contact me if you have any questions. What are the next steps? What do you need to do now to go forward?’ That has been a big change because all of a sudden it’s me and the patient working together as a team to get to their goals, not having to go through reception, wait for lunchtime, me to be too busy to call them back.
In this day and age people don’t actually want to be calling up all the time. I actually do tell them every time that after eleven o’clock I won’t reply and you’ll have to wait. But no one takes the mick, everyone respects that I have a private life and I’ve got my own things to be doing.
Dr. Payman Langroudi: Stuart? From the patient management perspective, are you treating your private patients differently in that respect? Are you giving your patients your number, your e-mail? What are you doing?
The swap from NHS to private and looking after people properly is time
Dr. Stuart Ray: I don’t give them my e-mail or my number. After hearing that it’s a great idea. For me the biggest thing, the swap from NHS to private and looking after people properly is time. it’s not always about having the most expensive and the most amazing equipment. It’s about sitting down and listening to what people say, listen to what they want. I think there’s a lot of treatment plans and a lot of treatments done which dentists are good at, so they push what they are good at and actually patients leave unfulfilled. Really it’s sitting down, listening, having a good chat and sometimes in very informal environment away from the surgery.
We have a patient consultation room, which our treatment coordinator uses as well. It’s actually quite nice to sit there with a coffee, especially for bigger treatment plans and just have a chat, nothing formal. And actually, when you’re in that relaxed environment, their true ‘wants’ come out far more easily than if you’re in a pressure clinical setting. For me that’s the biggest thing.
When you’re actually talking to a patient if they are in the dental chair, make sure you’re actually giving them eye contact. Don’t be looking around the room, don’t be sitting down, writing stuff down. Someone else can make notes if that’s what you need. I find that if you sit a little lower as well it means you’re not dominating and imposing yourself on the patient. Nervous patients are not hand on the shoulder. It’s reassurance. It’s old fashioned care. It’s old fashioned good manners and listening.
Dr. Payman Langroudi: You’ve been demonstrating on the Mini Smile Makeover course for the whole of last year, and Millie you’ve been helping us throughout AACD and the very beginning of the course. You see dentists going through this journey within two days, changing the way they look at anterior statics and becoming more minimally invasive. What are the most common things that you find time and time again that dentists are doing that you have to put right?
Dr. Stuart Ray: I think the most common issue I see is becoming very focused on looking down on a tooth. They lack the vision to look at all the different angles. And for me, what I have said a lot today is keep checking all your work. If it’s anterior work from an incisal perspective, it will give you the buccal palatal relationship. You can see the line angles, you can see all the reflective and deflective zones. For me it’s actually very simple. Don’t get too focused and too driven on looking down on a tooth, make sure you’re moving the head around and making sure you’re viewing it from all angles.
Dr. Payman Langroudi: That is a big one?
Dr. Stuart Ray: I think it’s huge. I think it’s amazing how a small adjustment made looking from the incisal can transform the look of a restoration, especially when you’re looking at line angle positioning. Thickness as well. It’s amazing how if you’re just half a millimeter too thick compared to the adjacent tooth it really does make it look far more dominant. I think that’s the biggest thing for me. Millie?
Dr. Millie Morrison: Yeah, I agree with that. In practice I’m always checking from each angle with my mirror, but also I get my nurse to be checking from her angle because where we sit and where the nurse is is completely different. Sometimes we get so focused that we miss something and it’s nice to get the the nurse’s point of view, because she’ll be able to see things differently. Also, involving her is good because when we’re brushing and then sculpting for an hour and a half, she’s like, “I want to have a nap, can I have a cup of tea?” Also the patient really enjoys you’re working as a team, and it’s not just the dentist doing it, you’re working together, you’re chatting a bit or discussing the work, and they really feel like they’re getting a tailor-made experience to them, which they really like.
Mistakes that people make – I think some people try to rush the beginning steps so then they can put in all this fancy secondary, tertiary anatomy. What happens is because they don’t focus on the basics to begin with, by the time we get to the finishing and polishing it’s not quite right.
Dr. Payman Langroudi: Each step is predicated on the one before, right?
Dr. Millie Morrison: Exactly, there’s no rushing through. It’s almost taking a moment, sitting back, looking at each step and every single angle, making sure you’re happy before moving on and having that discipline to check in with yourself, checking in with the nurse and then going forward.
Dr. Payman Langroudi: I think for me though, we’ve been on this course so many times, we’ve listened to Dipesh so many times, we take it for granted, the different materials, where they go, their physical and optical properties. I find on the course people have to get used to these words and they’re not necessarily new words, we’re talking micro hybrid, nano fill, micro fill.
Because most dentists just use a tube of composite, they’re not even thinking on what’s that material can do for them. I think the biggest disconnect is that we take some of that for granted, and even though someone’s been told once, it’s taken me 50 times to get to this stage. It’s something that as a teacher in this situation you’ve got to be aware of; even though it’s been on the screen, it does need repetition, it is huge.
Dr. Millie Morrison: I completely agree. When I first started being involved and learning about different types of composite material my head almost exploded because there was so much information I needed to take in and then apply.
Dr. Payman Langroudi: Whereas actually it’s very simple.
Dr. Millie Morrison: Yeah, it’s so simple, but you’re coming at it from a completely different point of view, and that’s why it’s even more important to take each step, so you’re fully understanding what you’re doing and what you’re trying to achieve.
Dr. Payman Langroudi: We can see it in the three exercises. Everyone’s getting progressively better and on the third one everyone’s doing amazing work. For me that’s a lovely thing.
Dr. Stuart Ray: Today I think it’s been absolutely mind blowing, quite honestly. Some of the work that’s been produced today I’m actually wondering whether these people have done this course four or five times, it’s that good. I’m really impressed. I think that’s where Dipesh’s teaching comes in as well, because it’s all about keeping things simple. If you over complicate everything, there’s so much to learn, you won’t learn anything. Your mind will just ignore the half of it, so I think simplicity is definitely the key.
Better is the enemy of best
From what you were saying about involving nurses and things like that, one thing I do is if I’m messing about with things too much, I make sure she gives me a good kick under the chair. One of the most important lessons I’ve ever been told is that better is the enemy of best. You do your best, you try and make things better and better, and invariably it gets far worse. Sometimes you need to stop and take a step back.
Dr. Payman Langroudi: We talk about it at Enlighten all the time, perfection paralysis. When I was a dentist, one thing I used to do was to phone up all my patients every day. I was getting fantastic results from that. People were amazed that the dentists was phoning them up. Then I thought, I’m only gonna phone up three a day, which three is that going to be? Maybe it would be the RCT, the extraction or whatever.
Coming back to your point on nurses, I said to the nurse, you decide who to call and you call. Firstly, it made my job easier, but secondly, her involvement in that and the appreciation from the patient that the practice had called them (she would say, “Dr. Langroudi wants to know if you’re okay”), the patient would always be surprised and happy. The fact that she’d chosen them, she’d called them and she’d come back… we wouldn’t even talk about it unless there was an issue. But she would constantly come back to me and say, Mr. so and so was happy to hear from us.
I gave up eight years ago, and still a lot of people don’t call their patients. It’s such a simple thing to do, call your patients afterwards. We were talking about calling your patients before their first visit. No one does that, and it’s such a good idea. You’re going to a new place, you know what to expect. Your dentist calls you before you arrive to find out whether there’s anything you’re worried about, and there’s always a few things you’re worried about, whether it’s cost, pain etc. It’s such a simple thing.
Dr. Stuart Ray: Do you think it’s best for the dentist to do that? What about a treatment care coordinator?
Dr. Payman Langroudi: I think the ideal situation for the dentist is to do it. But if you’re getting a 100 patients a month, maybe the dentist doesn’t want to do it and you’ll have to outsource it to the rest of the team.
Dr. Stuart Ray: Again, it’s going back to the old fashioned values, isn’t it? Trying to look after people and not look at the teeth as a source of income, but unfortunately some people only focus on that. A lot of the new patients I see in our practice is because people are completely unhappy with the service they’ve been offered; not with the dentistry, but with the service.
Often you pick your surgeon based on who you get on with the most, and it makes no sense at all
Dr. Payman Langroudi: I don’t know if you guys have ever been involved with surgeons (hopefully not), but often you pick your surgeon based on who you get on with the most, and it makes no sense at all.
Dr. Millie Morrison: If I’m doing a multi-discipline case and I know that they’ve got their surgery on Wednesday, then I set reminders for myself through the SOE software to email or text them.
Dr. Payman Langroudi: Before or after?
Dr. Millie Morrison: After. And I would just say, “how did your surgery go yesterday?”
Dr. Payman Langroudi: Before would be even better.
Dr. Millie Morrison: But it’s not with me… an implant has been placed, there has been a crown lengthening or they’re having a root canal with the specialist and I just might e-mail them afterwards. So it’s coming back to the fact that you’re going to see the specialist for this this particular point in treatment, but I’m adding value to myself as the restorative dentist because you (the patient) are coming back to me and I’m maintaining that relationship.
Dr. Payman Langroudi: Very nice. Well, time’s caught up with us. I want to thank you guys for the last couple of days.
Dr. Millie Morrison: Thank you.
Dr. Stuart Ray: Thank you for having us.
› DIG DEEPER ‹
» eBooks
Read up on the 6 tips that will perfect your anterior resin restorations here.
And to discover how you can achieve the aesthetic results you want when doing a single veneer with a single shade of composite, click here.
» Websites
If you want to learn more about the 2-day hands-on anterior composite masterclass with Dr Dipesh Parmar, click here.

» Training
To become an Enlighten Whitening Expert and get CPD certified for free hit the button below to take our hour-long online training.
» eBooks
Learn how to dramatically increase the number of whitening treatments you do here.
» Websites
Or if you’re interested in knowing more about the Enlighten Teeth Whitening System, then give it a click right here.
» Podcast
Learn how to emulate the success of the movers and shakers in the dental industry from their own mouths, featuring the nuggets of knowledge from likes of Simon Chard, Andrew Moore, Tif Qureshi, Mark Hughes and many more.