M(I)Y Aesthetics
Incorporating minimally invasive principles in aesthetic management of fractured anterior teeth.
Maximum conservation of the affected tissues, which have the potential to heal and bounce back to normal health and function, is the core principle of the modern minimally invasive techniques. A care plan should always be devised considering the longevity of the tooth and not the restorative replacement. In a prepared tooth the size of the preparation is inversely proportional to the fracture strength of the tooth structure. Furthermore no restoration lasts a life time. Even a meticulous done restoration is pushed into a re-restoration cycle. Hence avoiding unnecessary large preparations is of paramount importance.
Developments and innovations in the field of material science are being extremely supportive in executing minimally invasive (MI) preparations of tooth. Over the years the aesthetic properties of direct restorative materials have been constantly evolving. Nanotechnology has played an important role in aesthetics by modifying the particle size of contemporary composites (ranging between 1-10nm) to match that of hydroxyapatite crystals. This helps in providing a blended interface between the tooth and material which is close to natural.
Certain systems use different combination of nano-fillers and pre-polymerised fillers to reduce polymerisation shrinkage, increase fracture resistance, and improve polishability and match the wear resistance to that of natural teeth (Trimodal technique used in Premise, Kerr Dental). Polychromatic materials aid in realistic replacement of lost surfaces of teeth. The colour and opacity of the material determines its clinical application. Overlaying resins with different compositions aid in achieving natural tooth like restorations with similar reflective and refractive properties. Most of the above-mentioned characteristics are incorporated into the contemporary materials available in the market.
Contemporary adhesive systems exhibit high degree of conversion in etched as well as smear layer laden substrate, thereby supporting MI preparations. The initiators play a key role in optimising the degree of conversion. Dual curing systems which contain both photo and chemically curing initiators are believed to boost the polymerisation and thereby increasing the degree of conversion. Adhesion promoting monomers like 4-MET, 10-MDP and MAC-10 have revolutionised the dental field by their ability to form ionic bonds with calcium.
Case presentation
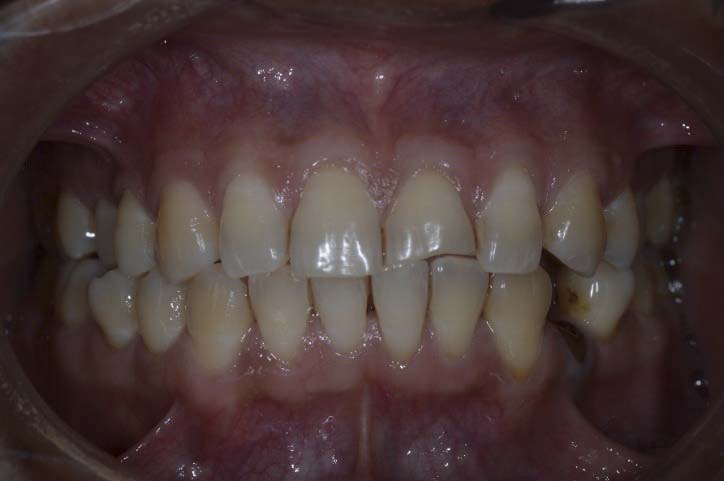
A 40 years old male, presented with a non-complicated traumatic fracture in left maxillary central incisor. The patient also reported that the tooth was asymptomatic since the day of fracture (approximately two years). He was concerned about his smile and looked forwarded for an aesthetic replacement for the lost fragment of the tooth.
Special test
Intra oral periapical X-ray was taken and sensibility tests were done to arrive at a confirmatory diagnosis.
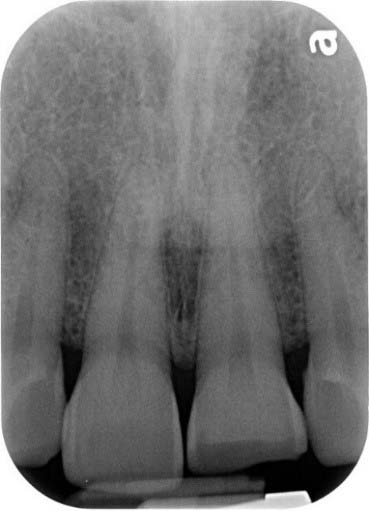
The fracture extends only upto D2 and no periapical changes have been detected.
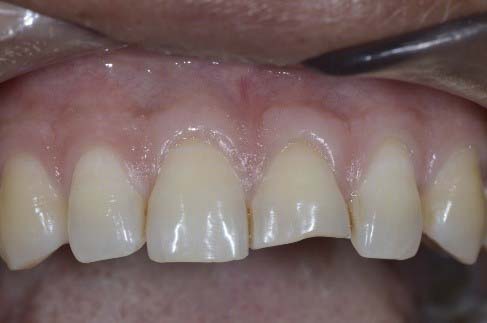
Sensibility test results of the affected tooth matched that of the control tooth confirming the absence of pulpal inflammation
Restorative care
Based on the special test results the decision was made to restore the tooth with resin composite. The reason being they provide good aesthetic results with acceptable longevity. When combined with minimal preparation the damage to the tooth would be negligible when compared to the other options. The physical properties of the resin also made it a suitable choice. Micro and Nano filled composites come in varying dentine and enamel shades along with staining resins which aid in creating perfect surface texture.
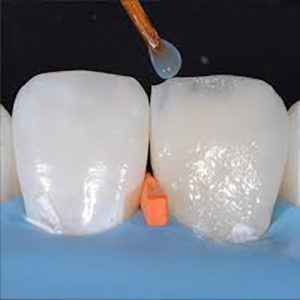
The first step in an aesthetic replacement of a fractured fragment of tooth is shade selection. Shade selection was done in ambient day light using a custom-made shade guide. Following shade selection isolation of the work field was accomplished using rubber dam. Fractured tooth was bevelled. Bevelling was followed by etching using 37% ortho phosphoric acid. Part of aprismatic enamel (cervical to the bevelled surface) was also etched to facilitate an aesthetic outcome (to avoid a demarcated border at the restoration and tooth interface). Adjacent teeth were protected by clear matrices during the process of etching. 7th Generation adhesive was applied onto the surface with a micro brush air dried for 5-10seconds and then was cured for 20 seconds.
Micro-Hybrid composite was used to restore the tooth. Layering technique was employed and flat plastic was the instrument used to place the composite and shape the restoration. Medium dentine and light enamel were layered to mimic the natural form and shade of the tooth. Gross carving was done with composite finishing burs and polishing was completed with Rainbow polishing disc and polishing paste.
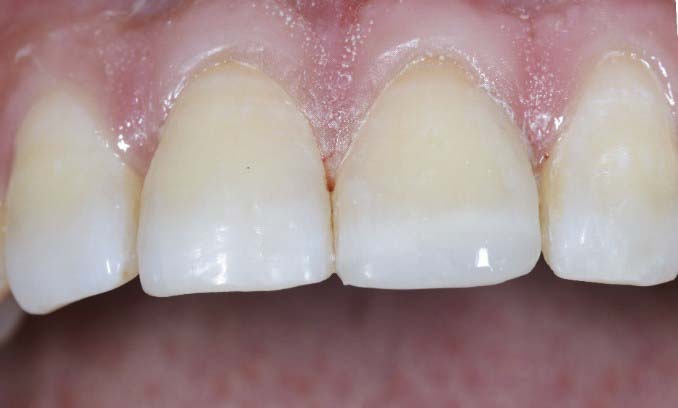
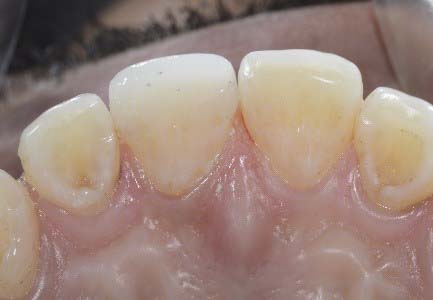
Why composites for M(I)Y restorative procedures
The main advantage of direct composites is that they require minimal tooth preparation for their placement. They are relatively pulp friendly and most amendable material, posing less challenges towards repair. Their wear resistance is comparable to that of natural teeth and hence they reduce the risk of tooth wear to the opposing/occluding teeth (when compared to the other available materials). Secondary and tertiary surface textures can also be incorporated within the restoration. They are generally completed in a single visit and hence do not demand the placement of provisional restorations. Despite yielding exquisite results these procedures are available at a low financial cost.
Never the less, these restorations also have some disadvantages which include, post-operative hypersensitivity, marginal discolouration, adhesive failure and reduced longevity. However, the material supports re furbishing and localised repair, which would aid in overcoming a few of the disadvantages.
Conclusion
Traditional restorative management of diseased/fractured teeth results in irreversible loss of dental hard tissues, which pushes them into a repetitive cycle of restoration and re-restoration which ultimately weaken teeth. MI management aims at maximum conservation of tooth structure, by employing minimally invasive operative procedures and utilising contemporary adhesive materials. However, the success of the treatment linearly relates to patient motivation and his/her understanding of the disease process and its management. Hence MI restorative treatments combined with appropriate patient education is the best way to manage teeth which require restorative care.
› DIG DEEPER ‹

» Training
To become an Enlighten Whitening Expert and get CPD certified for free hit the button below to take our hour-long online training.
» eBooks
Learn how to dramatically increase the number of whitening treatments you do here.
» Websites
Or if you’re interested in knowing more about the Enlighten Teeth Whitening System, then give it a click right here.
» eBooks
Read up on the 6 tips that will perfect your anterior resin restorations here.
And to discover how you can achieve the aesthetic results you want when doing a single veneer with a single shade of composite, click here.
» Websites
If you want to learn more about the 2-day hands-on anterior composite masterclass with Dr Dipesh Parmar, click here.
» Podcast
Learn how to emulate the success of the movers and shakers in the dental industry from their own mouths, featuring the nuggets of knowledge from likes of Simon Chard, Andrew Moore, Tif Qureshi, Mark Hughes and many more.